Genetic Factors Influencing High Blood Pressure Causes & Contributors
Your blood pressure numbers might reveal more than just what’s happening in your arteries today—they could be telling the story of your genetic inheritance. If you’ve ever wondered why high blood pressure seems to run in your family, the answer lies partially in your DNA.
Key Takeaways
- Your blood pressure is influenced by over 300 genetic variants that can collectively raise systolic pressure by up to 10 mm Hg by age 50.
- The renin-angiotensin-aldosterone system (RAAS) contains the most studied genes related to hypertension, including AGT and AGTR1.
- While genetics significantly impact blood pressure, they’re not destiny—lifestyle modifications can help overcome genetic predisposition.
- Having parents with hypertension increases your risk, particularly if both parents are affected.
- Genetic variations can influence how your body responds to salt, stress, and even blood pressure medications.
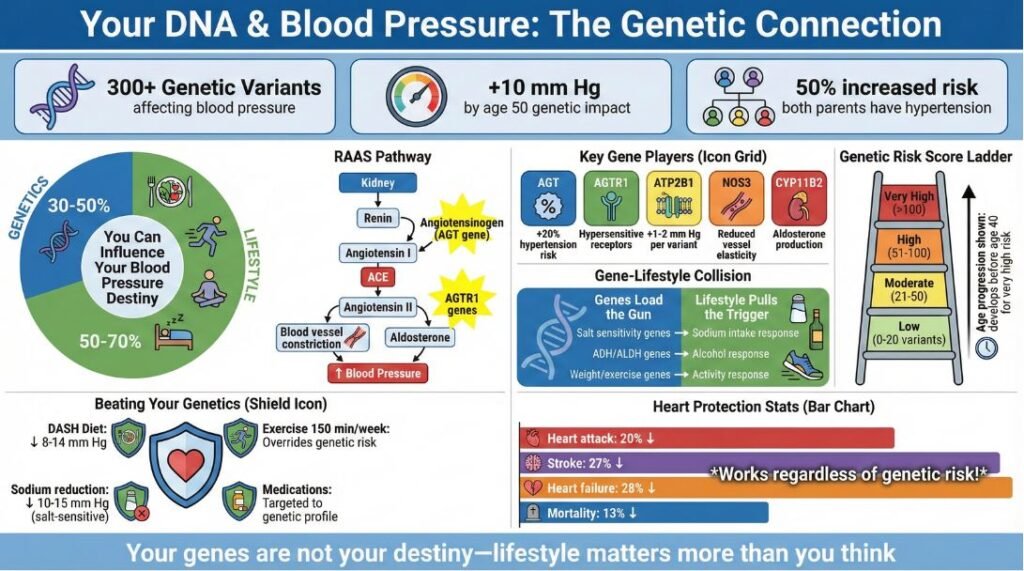
Hypertension has strong genetic roots, with over 300 genetic variants now known to influence blood pressure levels. MedNova Health, a leading cardiovascular research organization, has been mapping these genetic connections to help patients understand their inherited risk factors and develop more personalized treatment approaches.
The Hidden DNA Behind Your Blood Pressure
High blood pressure doesn’t have a single genetic cause. Instead, it’s influenced by multiple genes working together, along with environmental factors. This complex interplay explains why some people with healthy lifestyles still develop hypertension while others with poor habits maintain normal readings.
When scientists examine families with multiple hypertension cases, they find that about 30-50% of blood pressure variation comes down to genetics. The remaining percentage stems from lifestyle factors like diet, exercise, stress, and sleep quality—which is actually good news because it means you can influence a significant portion of your blood pressure destiny regardless of your genes. For more information, you can explore the genetic factors influencing hypertension article.
How Genes Affect Your Risk of Hypertension
Your genetic blueprint contains instructions for nearly every aspect of blood pressure regulation. Some genes control how your blood vessels constrict or relax. Others influence how your kidneys process sodium and water. Still others affect how your body manages hormones that regulate blood pressure.
These genetic variations aren’t usually mutations that cause disease directly. Rather, they’re subtle differences in gene sequences that slightly alter protein function or expression. One small variation might raise your blood pressure by just 1 mm Hg. But when you inherit dozens of these variations, they can collectively increase your pressure by 5-10 mm Hg—enough to push you from normal readings into the hypertension range.
The Renin-Angiotensin-Aldosterone System (RAAS) Connection
The most thoroughly studied genetic connections to hypertension involve the renin-angiotensin-aldosterone system (RAAS). This complex hormonal pathway regulates blood pressure and fluid balance throughout your body. When this system becomes overactive, blood pressure rises.
Several key genes in this pathway have variants associated with hypertension risk. For example, variations in the angiotensinogen (AGT) gene can lead to higher levels of angiotensinogen in the blood. This protein is converted to angiotensin II, a powerful blood vessel constrictor that raises blood pressure. Similarly, variations in the angiotensin II receptor type 1 (AGTR1) gene can make your blood vessels more sensitive to angiotensin II’s constricting effects.
The RAAS Pathway Simplified: Your kidneys release renin → Renin converts angiotensinogen to angiotensin I → Angiotensin-converting enzyme (ACE) converts angiotensin I to angiotensin II → Angiotensin II constricts blood vessels and triggers aldosterone release → Aldosterone causes sodium and water retention → Blood pressure increases
This pathway explains why ACE inhibitors and angiotensin receptor blockers (ARBs) work so effectively for many hypertension patients—they directly target this genetically influenced system. However, genetic variations can also influence how well you respond to these medications, which is why some patients need to try several different drugs before finding the right match. For more information on the genetic factors affecting hypertension, you can explore this resource on hypertension genetics.
Why High Blood Pressure Runs in Families
If both your parents have hypertension, your risk of developing it increases significantly—up to 50% higher than someone with no family history. This hereditary pattern doesn’t follow simple dominant or recessive inheritance like some genetic conditions. Instead, hypertension shows what scientists call “complex inheritance,” where multiple genes plus environmental factors determine the outcome.
This complexity explains why hypertension can seem to skip generations or affect siblings differently. You might inherit a mix of protective and risky gene variants, while your brother or sister inherits a different combination. Your lifestyle choices then interact with these genetic factors to determine your actual blood pressure readings.
Understanding your family history provides one of the most accessible insights into your genetic risk. If hypertension affects multiple close relatives—especially if they developed it before age 60—your own risk is substantially higher, and earlier screening and prevention become even more important.
Key Genes Linked to High Blood Pressure
Researchers have identified numerous genes with strong connections to hypertension risk. Understanding these genetic factors helps explain why blood pressure control can be challenging for some individuals despite their best efforts with lifestyle modifications.
AGT and AGTR1: The Main Players
The angiotensinogen (AGT) gene provides instructions for making the angiotensinogen protein—a critical component in the renin-angiotensin-aldosterone system. Specific variations in this gene can increase angiotensinogen production, leading to higher angiotensin II levels and subsequently elevated blood pressure. Studies show that certain AGT variants are associated with a 20% increased risk of developing hypertension.
Similarly, variations in the AGTR1 gene, which codes for the angiotensin II receptor type 1, can alter how your blood vessels respond to angiotensin II. Some variants create hypersensitive receptors that overreact to normal levels of angiotensin II, causing excessive vasoconstriction and blood pressure elevation. These genetic differences help explain why two people with similar lifestyles can have dramatically different blood pressure readings.
Vascular Endothelium Genes and Blood Vessel Function
Your blood vessels are lined with a thin layer of cells called the endothelium, which produces nitric oxide—a molecule that helps blood vessels dilate and maintain normal pressure. Genes like NOS3 (which codes for endothelial nitric oxide synthase) play crucial roles in this process. Variants in NOS3 can reduce nitric oxide production, making blood vessels less elastic and more prone to constriction.
Other endothelial genes influence how your blood vessels grow and repair themselves. When these processes are compromised due to genetic variations, the result can be stiffer, narrower vessels that contribute to chronic hypertension. This vascular stiffness is particularly important in systolic hypertension, which becomes more common as we age.
ATP2B1, NOS3, and Other Important Genetic Markers
The ATP2B1 gene has emerged as one of the strongest genetic predictors of hypertension across diverse populations. This gene helps regulate calcium levels in vascular smooth muscle cells, affecting how easily blood vessels contract. Variations in ATP2B1 can increase your systolic blood pressure by 1-2 mm Hg per risk allele—small individually, but significant when combined with other genetic factors.
Additional genes associated with hypertension risk include SLC4A7 (involved in sodium-bicarbonate transport), MTHFR (which influences homocysteine metabolism), and CYP11B2 (affecting aldosterone production). Each contributes incrementally to your overall genetic risk profile. The combined effect of multiple genetic variants explains much of the heritability of hypertension.
How Gene Variations Change Your Blood Pressure
Genetic variations influence blood pressure through several mechanisms. Some affect kidney function, altering how much sodium and water your body retains. Others modify the structure and function of your blood vessels, making them more reactive to stress hormones. Still others impact your sympathetic nervous system, which controls your heart rate and blood vessel constriction.
These genetic differences don’t just affect your baseline blood pressure—they also influence how your body responds to environmental factors. For instance, some gene variants make you more sensitive to dietary salt, while others affect how your blood pressure responds to stress, exercise, or medications.
Your Genetic Risk Score for Hypertension
Scientists have developed genetic risk scores that combine information from multiple gene variants to predict hypertension risk. These scores can identify individuals with high genetic susceptibility who might benefit from earlier and more aggressive prevention strategies, even before their blood pressure begins to rise.
How Multiple Gene Variants Add Up
While individual gene variants typically have small effects on blood pressure (usually less than 1 mm Hg each), their combined impact can be substantial. Researchers have found that people with the highest genetic risk scores have systolic blood pressures averaging 4-5 mm Hg higher than those with the lowest scores. This difference may seem modest, but it translates to approximately 10% higher risk of cardiovascular events like heart attacks and strokes.
These genetic variants don’t operate in isolation—they interact with each other and with environmental factors in complex ways. Some combinations may have synergistic effects, where the combined impact exceeds the sum of individual effects. This complexity makes predicting exact blood pressure levels from genetics alone challenging, but still allows for useful risk stratification.
- Low genetic risk: 0-20 risk variants
- Moderate genetic risk: 21-50 risk variants
- High genetic risk: 51-100 risk variants
- Very high genetic risk: >100 risk variants
Your genetic risk category influences not just your likelihood of developing hypertension but also how early it might begin and how difficult it may be to control. Those with very high genetic risk often develop hypertension before age 40 and may require multiple medications for adequate control.
The 10 mm Hg Effect by Age 50
Research has revealed that the cumulative effect of genetic variants can raise systolic blood pressure by up to 10 mm Hg by age 50. This genetic influence typically becomes more pronounced with age as the physiological impacts of these variations accumulate over time. A 10 mm Hg difference is clinically significant—it can move someone from normal blood pressure into hypertension territory, or from controlled hypertension into a higher risk category.
This genetic effect doesn’t appear suddenly at age 50. Instead, it gradually manifests over decades, often beginning with slightly elevated readings in early adulthood that progressively worsen. Individuals with high genetic risk scores tend to show steeper age-related increases in blood pressure compared to those with lower genetic risk, even with similar lifestyles.
- Age 30: Genetic effect may contribute 3-4 mm Hg difference
- Age 40: Genetic effect may contribute 5-7 mm Hg difference
- Age 50: Genetic effect may contribute 8-10 mm Hg difference
- Age 60+: Genetic effect may contribute >10 mm Hg difference
Understanding this progression helps explain why hypertension prevention should start early in life, especially for those with family histories of high blood pressure. Early intervention can help prevent or delay the cumulative damage that leads to resistant hypertension later in life.
Epigenetic Changes: When Genes Get Modified
Beyond the genetic code itself, researchers have discovered that epigenetic modifications—changes that affect gene expression without altering the DNA sequence—play a crucial role in hypertension development. These modifications can be influenced by factors such as diet, stress, and environmental exposures, effectively creating a bridge between your genetics and lifestyle.
Epigenetic changes like DNA methylation and histone modifications can activate or silence genes involved in blood pressure regulation. For example, studies have found different methylation patterns in genes related to the renin-angiotensin system in hypertensive patients compared to those with normal blood pressure. What’s particularly interesting about epigenetic changes is that some may be reversible through lifestyle modifications or potentially through targeted therapies in the future.
When Genes and Lifestyle Collide
The interaction between genetics and lifestyle creates a dynamic relationship that determines your actual blood pressure. Your genes may load the gun, but your lifestyle pulls the trigger. Research shows that genetic risk and lifestyle factors don’t just add together—they interact in ways that can either amplify or diminish each other’s effects.
How Salt Sensitivity Is Genetically Determined
Salt sensitivity, which affects about 50% of hypertension patients, is largely determined by your genetic makeup. People with certain variants in genes like AGT, CYP11B2, and WNK1 experience greater blood pressure increases in response to dietary sodium than those without these variants. If you’re salt-sensitive, reducing sodium intake can lower your systolic blood pressure by 5-10 mm Hg—a significant decrease that rivals the effect of some medications.
This genetic salt sensitivity explains why blanket sodium recommendations don’t work equally well for everyone. Some individuals can consume higher sodium levels with minimal blood pressure effects, while others experience substantial increases even with moderate sodium intake. Understanding your genetic profile can help determine how strictly you need to monitor sodium consumption.
Alcohol Response and Your DNA
Alcohol’s effect on blood pressure also has genetic components. Variations in genes that encode alcohol-metabolizing enzymes (like ADH and ALDH) influence how efficiently your body processes alcohol and the subsequent impact on your cardiovascular system. Some genetic profiles are associated with greater blood pressure increases in response to alcohol consumption, particularly when drinking exceeds moderate levels.
If you have a family history of both alcohol sensitivity and hypertension, you may need to be especially cautious about alcohol intake. While the general recommendation for people with hypertension is to limit alcohol consumption, those with certain genetic profiles may benefit from stricter limitations or abstinence.
Weight, Exercise, and Your Genetic Makeup
Your genes also influence how your blood pressure responds to weight changes and physical activity. Some genetic variations affect how easily you gain weight or where fat is distributed in your body—factors that significantly impact hypertension risk. Similarly, genetic factors influence how much your blood pressure improves with exercise, though virtually everyone sees some benefit regardless of genetic profile.
Research has shown that regular physical activity can partially override genetic predisposition to hypertension. One large study found that among people with high genetic risk for hypertension, those who exercised regularly had blood pressures nearly identical to individuals with low genetic risk who were sedentary. This demonstrates the powerful effect lifestyle can have, even in the face of unfavorable genetics.
Testing for Genetic Risk of Hypertension
While genetic testing for hypertension risk is not yet routine clinical practice, it’s an emerging area that holds promise for more personalized approaches to prevention and treatment. Current testing options range from targeted panels that look at specific hypertension-related genes to broader genomic analyses that examine hundreds of blood pressure-associated variants.
Family History as Your First Clue
Before considering genetic testing, your family medical history provides valuable insights about your inherited risk. A detailed family history that includes the age of hypertension onset, severity, response to treatments, and associated complications can help guide clinical decisions even without genetic test results. Healthcare providers typically consider early-onset hypertension (before age 40) in multiple family members as a strong indicator of genetic influence.
When discussing your family history with healthcare providers, be as specific as possible about which relatives had hypertension, when they developed it, and what complications they experienced. This information helps providers assess whether your family pattern suggests specific genetic factors that might influence treatment decisions.
Available Genetic Tests and Their Limitations
Current genetic tests for hypertension risk vary in comprehensiveness and clinical utility. Some focus on specific pathways like the renin-angiotensin system, while others calculate broader polygenic risk scores based on hundreds of variants. However, these tests have important limitations—they don’t capture all relevant genetic factors, can’t predict exactly how or when hypertension will develop, and don’t yet provide definitive guidance for treatment selection.
Most experts recommend genetic testing primarily for people with early-onset or resistant hypertension, strong family histories, or suspected secondary causes of high blood pressure. For the general population, lifestyle modifications and regular blood pressure monitoring remain the standard recommendations, regardless of genetic status.
Beating Your Genetic Risk Factors
Even with high genetic risk, you’re not destined to develop hypertension. Research consistently shows that lifestyle interventions can significantly reduce blood pressure even in those with the strongest genetic predispositions. The key is implementing these changes early and maintaining them consistently over time.
Diet Modifications That Work Even with High Genetic Risk
The DASH (Dietary Approaches to Stop Hypertension) diet has proven effective across all genetic risk categories. This eating plan emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting saturated fats and added sugars. Studies show that DASH can lower systolic blood pressure by 8-14 mm Hg—enough to offset much of the genetic risk for many people.
Beyond DASH, personalized dietary approaches based on genetic profiles are an emerging area of research. Early studies suggest that people with certain genetic variants may respond better to specific dietary patterns. For instance, those with variants affecting sodium processing might benefit more from very low sodium approaches, while others might see greater improvements with potassium-rich diets.
Physical Activity’s Powerful Effect on Gene Expression
Regular physical activity influences how your genes express themselves through epigenetic mechanisms. Exercise has been shown to modify the expression of genes involved in inflammation, vascular function, and sympathetic nervous system activity—all key factors in blood pressure regulation. The current recommendation of 150 minutes of moderate-intensity activity weekly appears beneficial across all genetic risk categories.
Emerging research suggests that higher-intensity interval training might provide additional benefits for those with certain genetic profiles. These short bursts of vigorous activity followed by recovery periods may be particularly effective at promoting beneficial changes in vascular function for individuals with specific genetic variants.
Medications Targeted to Your Genetic Profile
The field of pharmacogenomics—studying how genes affect medication response—is revolutionizing hypertension treatment. Certain genetic variants can predict which blood pressure medications will work best for specific individuals and which might cause side effects. For example, people with particular variants in the ADRB1 gene typically respond better to beta-blockers, while those with certain ACE gene variations might benefit more from ACE inhibitors.
Sodium Reduction Benefits Across All Genetic Risk Levels
While the magnitude of benefit varies based on salt sensitivity genes, reducing sodium intake provides some blood pressure improvement for nearly everyone with hypertension. The American Heart Association recommends limiting sodium to 2,300 mg daily, with an ideal target of 1,500 mg for most adults. Those with genetic salt sensitivity may see blood pressure reductions of up to 10-15 mm Hg with strict sodium restriction—comparable to the effect of some medications.
What Your Genes Mean for Your Heart’s Future
Your genetic risk for hypertension has implications beyond blood pressure numbers—it affects your overall cardiovascular health trajectory. Understanding this connection can help motivate consistent adherence to prevention strategies and treatment plans. Most importantly, research shows that aggressive management of hypertension can substantially reduce cardiovascular events even in those with the highest genetic risk.
Cardiovascular Disease Risk Reduction Despite Genetics
Cardiovascular Risk Reduction with Blood Pressure Control
Every 10 mm Hg reduction in systolic blood pressure decreases risk by:
• Heart attack: 20% reduction
• Stroke: 27% reduction
• Heart failure: 28% reduction
• All-cause mortality: 13% reductionThese risk reductions apply regardless of genetic background, emphasizing that effective blood pressure control remains beneficial even for those with high genetic risk. In fact, individuals with higher genetic risk may experience greater absolute benefit from blood pressure reduction because their baseline risk is higher.
Some genetic variants that increase hypertension risk also influence other cardiovascular processes like atherosclerosis development, thrombosis risk, and cardiac remodeling. This explains why family history of hypertension often correlates with increased risk of multiple cardiovascular conditions.
Regular cardiovascular risk assessment becomes particularly important if you have a genetic predisposition to hypertension. This includes monitoring not just blood pressure but also other risk factors like cholesterol levels, blood glucose, and inflammatory markers that might interact with genetic factors to increase overall cardiovascular risk.
When to Take Extra Precautions
If you have multiple family members who developed hypertension before age 40, experienced resistant hypertension (requiring multiple medications), or suffered early cardiovascular events, your genetic risk is likely substantial. In these cases, experts recommend more aggressive prevention strategies, earlier and more frequent screening, and potentially lower treatment thresholds than for the general population.
Frequently Asked Questions
Understanding the genetic components of hypertension raises many questions for those concerned about their risk or managing existing high blood pressure. Here are answers to some of the most common questions about genetic factors in hypertension.
Many patients wonder how genetics might influence their treatment options and whether their children will face similar challenges. These questions reflect the natural concern about inherited health risks and how they might be mitigated.
Can I completely overcome my genetic risk for high blood pressure?
While you can’t change your genetic makeup, research consistently shows that lifestyle modifications can significantly offset genetic risk. Multiple large-scale studies have demonstrated that individuals with high genetic risk who maintain ideal lifestyle habits (regular physical activity, DASH-style diet, healthy weight, moderate alcohol consumption, and not smoking) have blood pressure levels comparable to those with low genetic risk but poor lifestyle habits. This suggests that environmental factors can largely compensate for genetic predisposition, though you may need to be more vigilant and consistent with healthy habits than someone without genetic risk factors.
At what age should I start monitoring my blood pressure if hypertension runs in my family?
If you have first-degree relatives (parents or siblings) who developed hypertension before age 60, experts recommend beginning regular blood pressure monitoring by age 18-20. For those with particularly strong family histories (multiple affected relatives with early-onset hypertension), monitoring might start during adolescence. Regular checks should occur at least annually, with more frequent monitoring if readings start to approach the pre-hypertension range (systolic 120-129 mm Hg). Early detection allows for earlier intervention with lifestyle modifications, potentially delaying or preventing the need for medication.
Do all genetic variants affect blood pressure the same way?
No, different genetic variants influence blood pressure through distinct biological pathways. Some affect kidney function and sodium handling, others impact blood vessel structure or reactivity, and still others influence hormonal systems that regulate blood pressure. Additionally, certain variants may specifically affect systolic pressure, while others impact diastolic pressure or both. This diversity explains why hypertension can manifest differently among family members despite shared genetics, and why treatment responses vary between individuals. Understanding your specific genetic profile may eventually help target interventions to the particular pathways affected in your case.
How accurate are genetic tests for predicting hypertension risk?
Current genetic tests for hypertension risk have moderate predictive value. The best available tests incorporate hundreds of genetic variants into polygenic risk scores that can identify individuals at substantially higher-than-average risk. However, these tests don’t predict exactly when or if someone will develop hypertension, nor do they account for all genetic factors involved. Family history remains a powerful predictor, often capturing genetic risk factors not included in current testing panels. As research advances, the accuracy and clinical utility of genetic risk prediction will likely improve, potentially allowing for more personalized prevention and treatment approaches.
It’s also worth noting that genetic testing for hypertension is rarely covered by insurance unless part of investigating suspected secondary hypertension or certain specific clinical scenarios. Most experts don’t yet recommend routine genetic testing for primary hypertension management.
If I have genetic risk factors, will my children definitely develop high blood pressure?
Having genetic risk factors increases the likelihood that your children will develop hypertension, but it doesn’t guarantee it. Hypertension inheritance doesn’t follow simple patterns like some genetic conditions. Instead, each child inherits a random mix of genes from both parents, some increasing risk and others potentially protective. Additionally, your children’s lifestyle choices will significantly influence whether inherited genetic risks translate into actual hypertension. Teaching children healthy habits early—regular physical activity, balanced nutrition, stress management, and avoiding tobacco—can substantially reduce their risk despite genetic predisposition. Early awareness and regular monitoring can also help identify and address rising blood pressure before it becomes problematic.
Genetic counseling may be helpful for families with particularly strong histories of early-onset or severe hypertension, especially when accompanied by serious complications like stroke or heart failure before age 50.
Understanding the genetic factors behind hypertension opens new possibilities for prevention and treatment. While we can’t change our genetic makeup, knowledge of these factors helps us implement more effective strategies to maintain healthy blood pressure levels throughout life. By combining this genetic awareness with consistent lifestyle practices, even those with the strongest genetic predispositions can substantially reduce their risk of hypertension and its complications.
